Purpose
The purpose of this packet is to provide team members with education to assist in navigating the changes that have been at NMASCMG in response to the COVID-19 pandemic.
The following packet will include information on the following:
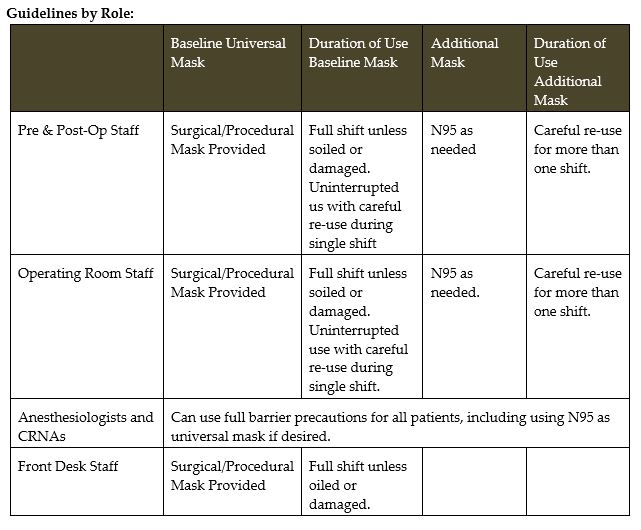
- Universal Masking – How to Wear & Guidelines
- Personal Protective Equipment (PPE)
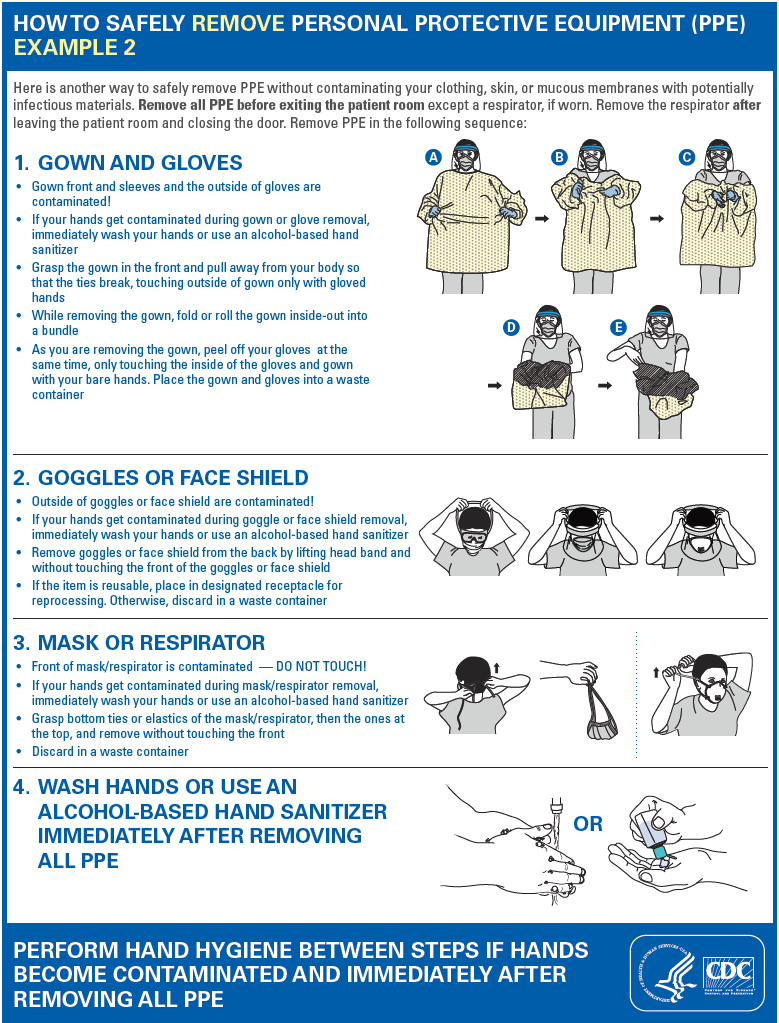
- Donning & Doffing
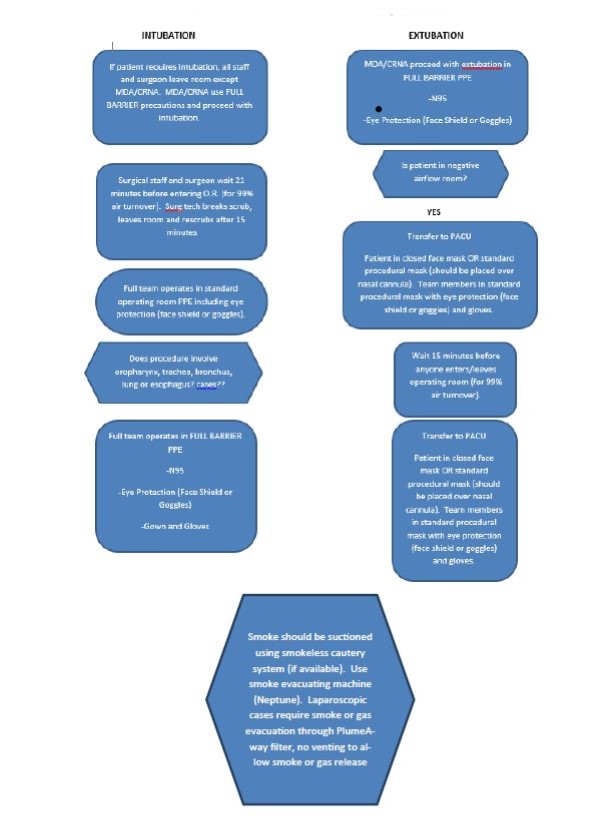
- Intubation/Extubation policy and practice
- Employee, physician and ancillary staff screening
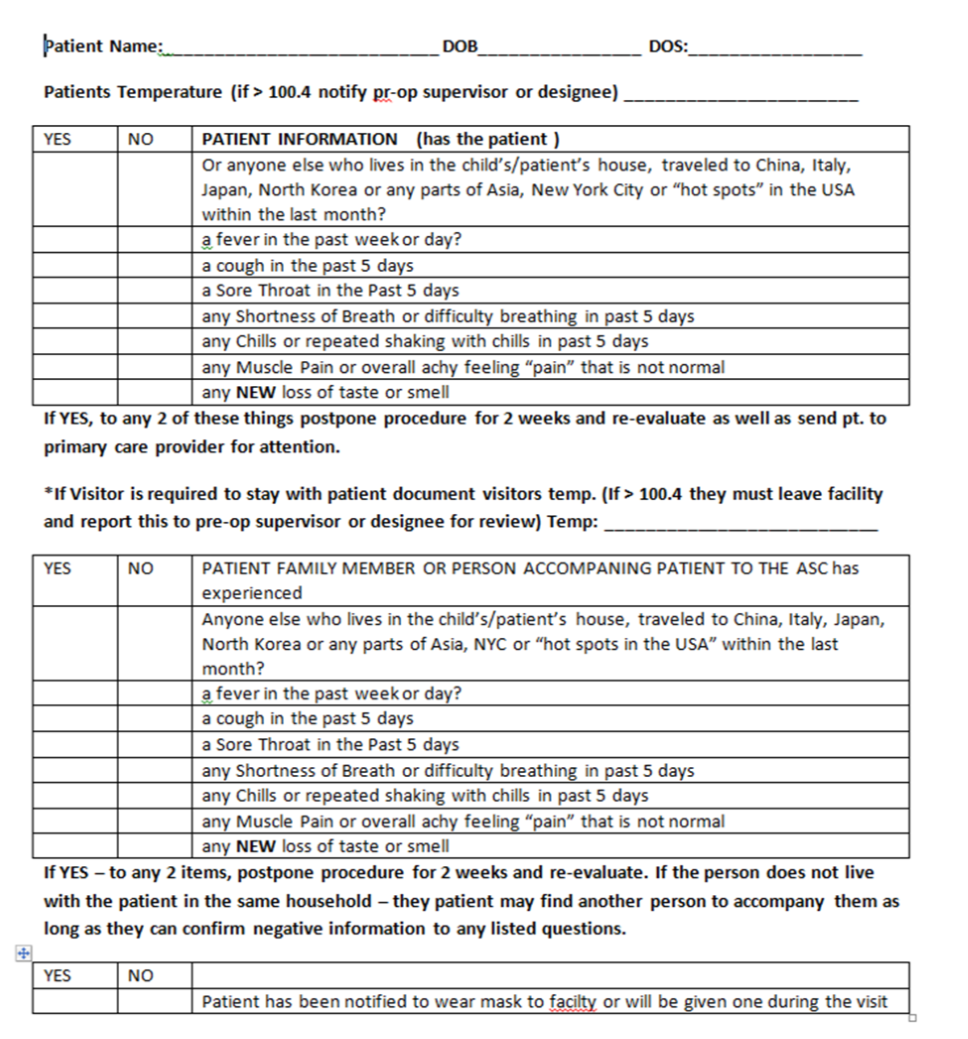
- Patient/Visitor screening
- Social Distancing while on break
- Environmental Cleaning
After reviewing this information, please communicate with the Clinical Director or departmental supervisors to ask and answer questions and be an ongoing advocate for infection prevention best practices in the ASC.
Goal
To provide guidance and education to our team for infection prevention questions/concerns and empower our team to actively problem solve issues utilizing our infection prevention created resources.
UNIVERSAL MASKING
The health of our team members while caring for patients remains a top priority. All team members must wear masks at all times while at work.
Definitions:
Uninterrupted Use: Uninterrupted use is the practice of wearing the same face mask or N95 for an extended period and for repeated close contact encounters with several different patients, without removing the face mask or N95 between patients. The expectation is that team members will wear the same face mask or N95 for their full shift. If the face mask or N95 respirator needs to be removed, team members should follow the careful reuse steps. Once you put a mask on, keep it for the entire shift unless soiled, damaged or hard to breathe through.
- Do not wear your mask around your chin or neck. You may contaminate on the OUTSIDE of your mask.
- For patients in droplet/contact or full barrier isolation, uninterrupted use and careful reuse of facemasks and N95 respirators is only acceptable if a barrier is present to shield from droplets.
Careful Use: Careful reuse involved removing your face mask or N95 as needed, placing it in a paper bag, and then donning again. Examples of when you would practice careful reuse:
- Team member moving between 2 patients, 1 requiring droplet/contact isolation (standard procedural mask), and another requiring full barrier isolation (N95 mask).
- Team member break requiring access to the nose or mouth.
Examples when you don’t reuse:
- When the mask becomes visibly soiled, wet, or damaged.
- The mask becomes hard to breathe through.
- At the end of a 12-hour shift.
How to Get Supplies
- PPE is stocked in normal locations. (gowns, gloves, shields, goggles).
- N95s must be obtained from manager and/or designated charge individual
- Procedural masks are allocated per department in the morning. Charge nurse/manager will bring to department in the morning.
- All team members will be provided one surgical/procedural face mask for your entire shift (up to 12 hours). N95/KN95 will be assigned to staff. Staff will have several masks assigned in order to allow for “dry out” and cleaning protocols ( see policy).
- A seal test must be performed by each team member upon donning their N95 mask. In the link below is a video on proper donning instructions and seal testing methods
- https://youtu.be/zNV6dK6Y-Ek
DONNING AND DOFFING
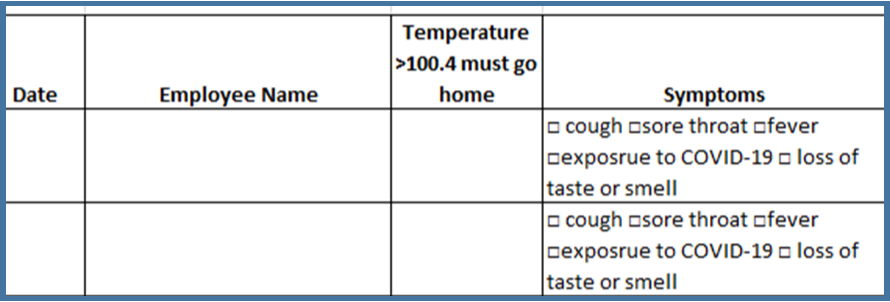
SCREENING:
All Staff, physicians, and other ancillary personnel MUST participate in daily screening of their temperature and symptom. All team members will wear a colored sticker with the date on it indicating to others that they have conducted the screening process. If any team member works greater than 6 hours they must rescreen.
All patients will be screened for signs, symptoms, exposure, and travel during the preoperative phone call. Patients will be notified that no one is allowed with them in the ASC unless the patient is a minor or a vulnerable adult. Post-operative care givers can wait in their vehicles and will receive a call when the procedure is complete. Physicians and staff can communicate with the post-operative care give via phone. Patients (and any visitors) will be screened before entering the ASC at a kiosk. A paper screening tool will be implemented upon check in at the newly developed screening kiosk and will be in the patients shadow chart.
PATIENT/VISITOR SCREENING
SOCIAL DISTANCING WHILE AT WORK:
In an attempt to reduce team member’s exposure we ask that everyone adhere to distancing, hand, and respiratory hygiene while on break. Furniture has been removed to allow for more adequate distancing in the breakroom. We encourage team members to utilize the atrium and other spaces during break time allowing for adequate distancing.
ENVIRONMENTAL CLEANING:
Strict adherence to our routine environmental cleaning should be followed. Close attention to cleaning items that are used for multiple patients typically classified as non-critical items, should be adhered to (B/P cuffs, pulse oximeter cords and probes, EKG cables, chairs, carts, bedside tables, etc.). Cleaning should take place in the OR AFTER the patient has left the OR and all trash including anesthesia trash, has been removed.
Q&A:
What is community exposure?
Community exposure may occur if you interact with a person that is ill with COVID-19. This is more likely to occur in areas that are experiencing sustained community transmission. The risk of contracting the infection is dependent upon the duration, frequency and proximity of exposure.
What are the quarantine expectations following personal travel?
We are following guidance from the CDC regarding restrictions following travel to Level 2 and Level 3 countries as well as cruises. You will be asked to disclose your travel to work and you may be asked to self-quarantine for 14 days, based on your exposure and current CDC guidance.
How do I self-disclose travel or potential community exposure?
Team members are asked to self-disclose any actual or potential exposure, including any travel to CDC identified high risk areas. Team members are asked to not return to work prior to this disclosure and assessment with a manager.
Where do I find the most recent testing guidelines?
The Minnesota Department of Health will be consulted for the most recent testing guidelines.
Will I be wearing a mask while at work?
Yes, we are implementing Universal Masking to help protect team members from community spread of COVID-19. This means that it is recommended that you will wear face masks at all times while at work. While universal masking is not mandatory at this time, we are strongly recommending it to protect our team members and patients.
What happens if I am exposed to COVID-19 at work?
All suspected workplace exposures should be reported to your manager immediately for evaluation.
How do I know if I have been exposed at work?
Every patient is instructed to phone the ASC within 14 days after the patient’s date of surgery to inform us if he or she has tested positive for COVID-19 or are experiencing any symptoms. Manager and/or designee will follow appropriate direction from our State Department of Health.
What happens if I am exposed at work and become ill with COVID-19?
If you contract COVID-19 due to an occupational exposure, this will generate a Worker’s Compensation claim and coverage will be determined by our carrier. We will compensate you for lost wages during the period of quarantine for work-related exposures.